Abstract
Despite distribution of millions of free mosquito nets in Angola, malaria remains the primary cause of mortality in young children, accounting for 35% of deaths among children under five (CU5). Our objectives were first to examine the association between malaria knowledge and bednet use for CU5, and second, to investigate the impact of multivariable logistic regression to analyze responses from a representative sample of women aged 15–49 from the Angola Malaria Indicator Survey (2011). Approximately 44% of respondents with CU5 (n=6,576) owned at least one bednet for sleeping, and of those 87.4% identified mosquitos as a cause of malaria. Adjusting for respondents’ age, region, and education, those reporting mosquitos as a cause of malaria had 1.7 (95%CI: 1.3–2.2) times the odds of bednet use for CU5 compared to those not reporting mosquitos as a malaria cause. Exposure to behaviour change communication (i.e. malaria messaging) increased the odds of bednet use where messaging encouraged sleeping under mosquito nets (OR: 1.3, 95%CI: 0.9–1.7). This study provides evidence of a positive association between malaria knowledge and bednet use, indicating that along with widescale distribution of bednets for malaria prevention, public health efforts in Angola should focus on increasing awareness and promoting bednet usage through targeted risk communication.
Introduction
Malaria is the primary cause of mortality in Angola and is the diagnosis of half of all patients in Angolan hospitals (Cosep Consultoria, Consaúde, and ICF International, 2012; Somandjinga, Lluberas, & Jobin, 2009). Over two million cases of malaria arise annually in Angola, and with only eight physicians per 100,000 people, treatment is extremely difficult (World Health Organization, 2011, 2015). Malaria studies in Angola use malaria prevalence to define four geographic regions, which include Hyperendemic, Mesoendemic Stable, Mesoendemic Unstable and the capital city of Luanda. Disparity exists between Luanda and the rest of the country in treatment of this disease. In Luanda, 26% of children were treated with antimalarial drugs compared to only 8% in the Hyperendemic region and 9% in the Mesoendemic Unstable region (Cosep Consultoria, Consaúde, and ICF International, 2012). Furthermore, extreme poverty and the lack of government infrastructure in Angola make treatment inaccessible, and further exacerbates the issue. Despite the influx of wealth into the country through oil production, only approximately $1 USD per capita of Angola’s national budget is allotted for malaria control (USAID, 2016). There is a need for the implementation of inexpensive preventative and control strategies against malaria in Angola to better overall national healthcare.
Malaria is an infectious disease caused by a parasite transmitted to humans through the bites of an infected mosquito (World Health Organization, 2015). Bednets are a low-cost, low-tech means of malaria prevention – acting as a physical barrier against mosquitos while sleeping. Malaria-carrying mosquitos feed predominantly at night, and therefore the use of bednets has the potential to greatly limit transmission to humans (Bayoh et al., 2014). A study in Kenya found an increase in bednet ownership and use correlated with an 85% reduction of indoor mosquito densities over a 10-year period (Mutuku et al., 2011). Bednets are available as insecticide-treated and untreated, and while insecticide-treated bednets kill mosquitos on contact, untreated bednets are sufficient as an obstruction to reduce the likelihood of mosquito bites (Mutuku et al., 2011). Bednet costs are low with median prices estimated at $5 USD (Walker, Griffin, Ferguson, & Ghani, 2016).
Malaria in children represent a significant burden of disease in Angola, and accounts for an estimated 35% of mortality in children under five (USAID, 2016). Young children often do not exhibit the typical signs and symptoms of malaria. Instead the disease presents similarly to gastroenteritis, meningitis, or pneumonia, leading to missed opportunities for treatment as detection is often too late, and making children extremely vulnerable to serious malaria infection (Schumacher & Spinelli, 2012). In Angola, a prevention-based method of malaria control through the distribution of free bednets was adopted in 2001. However, uptake has been slow and less than 30% of children under five (CU5) sleep under bednets after a decade of targeted bednet distribution (Cosep Consultoria, Consaúde, and ICF International, 2012; World Health Organization, 2015). Reasons for the low adoption rate are not well understood, and to the best of our knowledge no studies examining CU5 bednet use and malaria knowledge have been conducted in Angola. To gain insight into malaria bednet use in the context of knowledge and understanding of mosquitos as a vector for the disease we used the most recently available Angola Malaria Indicator Survey (2011) and investigated the association between knowledge of malaria cause and bednet use for CU5. The distribution of bednets has been accompanied by education campaigns using various formats such as radio, newspapers, brochures, health promoters etc., and consequently, we were also interested in the influence of malaria messaging on CU5 bednet use and examined this relationship for respondents who had seen or heard particular malaria messages.
Methods
Study designThe Angola Malaria Indicator Survey (AMIS) 2011 was conducted by Cosep Consultoria, Consaúde Lda., and the Programa Nacional de Controle da Malária, and implemented by ICF International under contract with USAID (Cosep Consultoria, Consaúde, and ICF International, 2012). This cross-sectional national survey was conducted from mid-January 2011 through May 2011 and collected data from women aged 15–49, including usual residents and persons staying in the household the night before the interviews were conducted. A multistage randomized cluster sampling methodology was employed and was representative of 8,030 households sampled across the 18 provinces in Angola that had been classified into one of three regional domains depending on the prevalence of malaria in the region: Hyperendemic, Mesoendemic Stable, and Mesoendemic Unstable. The Angolan capital, Luanda, was separated into its own region. In-person interviews were conducted on 8,589 eligible women, yielding a response rate of 98%. A detailed description of the sampling design and interview methods are available in the final report (Cosep Consultoria, Consaúde, and ICF International, 2012).
Analytic sample
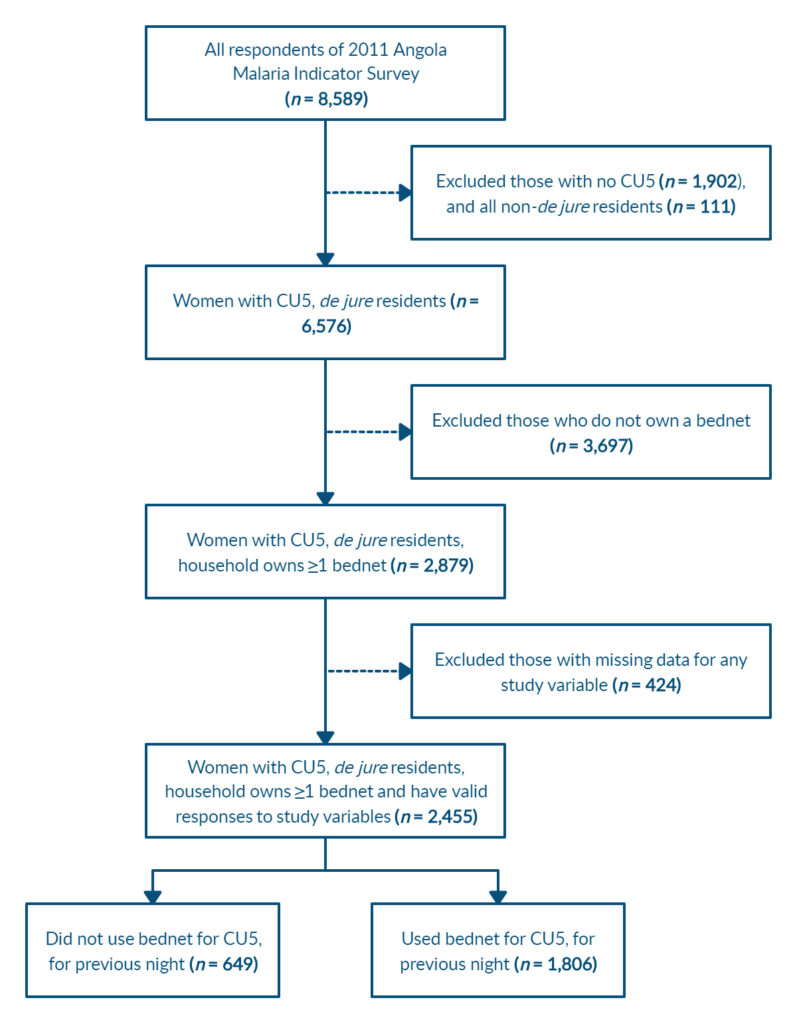
To examine the association between correct malaria knowledge and use of bednets for CU5 we analyzed responses from women aged 15–49 with complete data for all survey variables. Of the 8,589 AMIS respondents, those who were not de jure residents were excluded (n = 111), as well as those with no children under the age of five (n = 1,902), individuals living in households not owning at least one bednet (n = 3,697), and individuals with missing data for any study variables (n = 424). The final sample consisted of 2,455 respondents meeting inclusion criteria and providing valid responses to study variables (Figure 1).
Study variables
The dichotomous outcome variable of bednet use for CU5 (yes/no) was taken from the question “Did your child under 5 sleep under a bednet the previous night?”. Correct knowledge of malaria transmission was determined using self-reported data and derived from responses to the question “What causes malaria?”. Possible answers included: “Mosquitos”, “Dirty water”, “Dirty surroundings”, “Contaminated food”, “Witchcraft”, “Other”, and “Does not know any”. These responses, with the exception of “Does not know any”, were not mutually exclusive – respondents could indicate more than one cause of malaria. A dichotomous variable for correct knowledge (yes/no) was created by considering any incorrect response as No, and Yes where respondents indicated “Mosquitos” cause malaria.
Potential confounders to the relationship between malaria transmission knowledge and bednet use for CU5 were identified a priori and included: mother’s age (5-year age groupings), region (Hyperendemic, Mesoendemic Stable, Mesoendemic Unstable, Luanda), and highest level of education completed (no education, primary education, secondary education or higher). To determine the influence of malaria messaging – targeted communications as part of the bednet distribution campaign – on the use of bednets for CU5 we selected women in the analytic sample who indicated Yes to the question “In the past few months, have you seen or heard any messages about malaria?” (n = 1,218). We analyzed the Yes/No responses for two of the options provided (“Sleep under mosquito nets” and “Malaria kills”) to the question “What messages about malaria have you seen or heard?”.
Statistical analysis
Descriptive statistics were calculated for the analytic sample by the respondent’s age, region of residence, and educational background. Those excluded from the study due to missing responses were compared to those remaining in the analytic sample using chi-square tests to assess potential bias due to missing data. To examine the relationship between correct malaria transmission knowledge and bednet use for CU5 we performed multivariable logistic regression estimating the odds ratio (OR), adjusted OR (ORadjusted) and 95% confidence interval (CI). To investigate the robustness of the model to analytic assumptions, an additional analysis was conducted in which a multivariable model was constructed to separate the effects of multiple responses to the question of malaria causes (given that they were not mutually exclusive). All analyses were performed using SAS, University Edition (SAS Institute Inc., Cary, NC), and probability sampling weights provided by AMIS (2011) were applied to all analyses to account for the unequal probabilities of selection and nonresponse (Cosep Consultoria, Consaúde, and ICF International, 2012).
Ethics
The survey protocol was submitted to and approved by the Ethical Review Committee at the National Malaria Control Program and the Institutional Review Board (IRB) of Macro International. Verbal informed consent was obtained from all respondents participating in the survey.
Results
Of the 6,576 de jure AMIS respondents aged 15–49 with children under five, the relative frequency of bednet ownership was 44.1%. Excluding 424 respondents with missing data for any of the study variables, the resulting sample size was 2,455 women (Figure 1). Compared with respondents who remained in the analytical sample those excluded did not differ significantly in the women’s age group but were more likely to reside in the Hyperendemic or Mesoendemic Unstable regions (p < 0.0001) and have no education (p < 0.001).
Table 1 shows the demographics of the overall study sample, as well as the two groups defined by our outcome variable – those women that correctly identified “Mosquito bites” as the cause of malaria and those choosing any of the other possible responses seen in Table 2, except “Mosquito bites”. Approximately half of the study sample was under the age of 25. All four malaria epidemiologic regions were represented; however, the highest proportion of respondents resided in the Mesoendemic stable region (40.7%). The majority of respondents had attained only a primary education (64.3%).
Among those in the analytic sample owning one or more bednet, 74.2% indicated that CU5 slept under a bednet the previous night. The frequency of bednet use for CU5 was highest in respondents aged 20–24, those living in the Mesoendemic Stable region, and those with no education.
Malaria causes
When asked the survey question “What causes malaria?”, the largest proportion (87.4%) of respondents chose “Mosquito bites” of the seven options provided to them (Table 2). Other possible answers, such as “Dirty needle” or “Contaminated food”, represented 1.4%–34.7% of responses. To estimate the effect size for the association between correct malaria knowledge and bednet use for CU5, we used multivariable logistic regression (Table 3), and found increased odds of CU5 bednet use when women had correctly identified “Mosquito bites” as the cause of malaria, with an unadjusted odds ratio (OR) of 1.6 (95%CI: 1.2–2.1). After adjusting for age, region of residence, and education, we found an OR of 1.7 (95%CI: 1.3–2.2).
Compared to the oldest age group (45–49), all ages had increased odds of bednet use for CU5 with correct knowledge of malaria transmission, with the exception of women aged 40–44. We also found an increased odds for residents of all three malaria epidemiologic regions compared to Luanda, with those in the Mesoendemic Stable region having nearly two times the odds of bednet use for CU5 when respondents identified “Mosquito bites” as the cause of malaria. Women with primary level education or less had increased odds of bednet use for CU5 with correct malaria knowledge compared to respondents who achieved secondary or higher education. Because the AMIS survey permits respondents to select multiple responses to the question regarding the cause of malaria, we investigated how these multiple responses might affect our conclusions. We redefined the explanatory variable, adding a Maybe category to capture the respondents who selected “Mosquito bites” in addition to any of the other five possible causes of malaria. The main effect estimate for the redefined Yes category yielded a marginally higher odds ratio of 2.0 (95%CI: 1.5–2.6), and the new category of Maybe returned a marginally lower odds 1.4 (1.1–1.9) of bednet use for CU5.
Malaria messaging
Only 49.9% (n = 1,218) of women indicated they had seen or heard messaging (any media format e.g. radio, newspaper) regarding malaria. Of these women, 56.2% (n = 660) received messages to “Sleep under mosquito nets”, and even less (37.3%) had seen or heard messages indicating that “Malaria kills”. We found that the odds of bednet use for CU5 was increased for respondents indicating that they had seen or heard messaging regarding the use of mosquito nets, whereas the odds of bednet use for CU5 was decreased for those who had received messages that malaria kills; however, the 95% CI crossed ‘1’ in both instances (Table 4).
Discussion
The present study utilized the Angola Malaria Indicator Survey (2011), with data collected from more than 8,500 women, to investigate the relationship between knowledge of malaria transmission and use of bednets for children under five (CU5). Our study demonstrated in a representative population-based sample that correctly identifying mosquito bites as a cause of malaria was independently associated with an increased odds of bednet use for CU5 (ORadjusted 1.7, 95%CI: 1.3–2.2), and recent malaria messaging had little if any impact on use of bednets for CU5.
Our finding that correct knowledge of malaria transmission positively correlated to bednet use is consistent with studies conducted in other malaria-endemic countries in which malaria knowledge was assessed (García-Basteiro et al., 2011; Hwang et al., 2010), and our analysis yielded a nearly identical adjusted odds ratio – lending support to our conclusions. Additionally, we found those residing in any malaria-endemic region of Angola had increased odds of bednet use for CU5 with correct understanding that mosquito bites cause malaria compared to the capital of Luanda. This may be the result of targeted free bednet distribution in these regions and the information, education and communication strategies that have been paired with distribution (USAID, 2016). Yet, when examining the data collected around behavior change communication i.e. malaria messaging, delivered as part of the bednet distribution campaign, the results were mixed. Those that received information to sleep under mosquito nets had increased odds of bednet use, whereas those that had heard or seen messages that malaria can cause death had lower odds of bednet use for CU5. This is in contrast to a study in Ghana examining malaria messaging in which participants had more than three times the odds of bednet use in CU5 when they had received information regarding malaria (Owusu Adjah & Panayiotou, 2014). However, they did not analyze messages individually and may not be directly comparable to our findings.
The national sampling methodology of the AMIS resulted in a large survey dataset representative of the Angolan population and is a strength of this study. However, two important limitations should be discussed. First, the data was self-reported and due to social desirability respondents may have falsely stated to the interviewer that CU5 had slept under a bednet the previous night. If more respondents with correct knowledge of malaria transmission incorrectly reported bednet use this would have resulted in an overestimate in the odds ratios we observed. Given the survey questions were adapted to the local situation and interviewers were fully trained (Cosep Consultoria, Consaúde, and ICF International, 2012), we expect this to be limited; however, it cannot be dismissed as a source of bias. Second, the question of bednet use for CU5 was restricted to use the previous night. While reducing issues of recall, the response to this question does not represent regular use and may limit the generalizability of our findings with respect to consistent bednet usage. It should be noted that studies in which information was collected for both regular use of bednets as well as the previous nights’ use have found similar proportions among study participants (Animut et al., 2008; Xu, Liao, Liu, Nie, & Havumaki, 2014). Despite these limitations, this study provides the first evidence on the use of bednets for Angolan CU5 in association with knowledge of malaria transmission and indicates that understanding mosquitos are associated with malaria may increase bednet use. Yet, in spite of mass distribution campaigns that have included information and education regarding malaria, our findings suggest that the current communication on malaria risk have had little effect in promoting bednet use for CU5. The Precaution Adoption Process Model (PAPM) describes stages of health-related behaviour adoption – from being unaware of an issue (stage 1), to aware but unengaged (stage 2) through maintaining a health behaviour (stage 7), and provides a framework to develop risk communication strategies focused on changing perceptions and encouraging uptake of preventive health behaviours (Weinstein, 1988). Here, the desired action is use of bednets for young children. With nearly a quarter of respondents owning but not using a bednet for CU5, and more than half of respondents indicating they had not heard the message that “Malaria kills” it is likely that a significant proportion of individuals remain in stages 1 or 2. To increase awareness and ensure messages address specific beliefs and attitudes of a population, additional research is needed to determine the best delivery format.
In conclusion, findings from our study suggest there is a considerable gap between bednet ownership and use for CU5. Correct knowledge of malaria transmission through mosquito bites was associated with increased odds of CU5 sleeping under a bednet the previous night. With bednet ownership at less than 50% of households surveyed it is imperative that free bednet distribution campaigns continue. However, our findings with respect to malaria messaging indicate more work may be needed in this regard as it is important to not only increase the availability of bednets but ensure their use through increased awareness of the preventive steps that can be taken to protect those at highest risk.
References
- Animut, A., Gebre-Michael, T., Medhin, G., Balkew, M., Bashaye, S., & Seyoum, A. (2008). Assessment of Distribution, Knowledge and Utilization of Insecticide Treated Nets in Selected Malaria Prone Areas of Ethi-opia. The Ethiopian Journal of Health Development (EJHD), 22(3). Retrieved from http://www.ejhd.org/index.php/ejhd/article/view/511
- Bayoh, M. N., Walker, E. D., Kosgei, J., Ombok, M., Ol-ang, G. B., Githeko, A. K., … Gimnig, J. E. (2014). Persistently high estimates of late night, indoor exposure to malaria vectors despite high coverage of insecticide treated nets. Parasites & Vectors, 7, 380. https://doi. org/10.1186/1756-3305-7-380
- Cosep Consultoria, Consaúde, and ICF International. (2012). Angola Malaria Indicator Survey 2011. Calver-ton, Maryland: Cosep Consultoria, Consaúde, and ICF International. Retrieved from https://dhsprogram.com/pubs/pdf/MIS11/MIS11.pdf
- García-Basteiro, A. L., Schwabe, C., Aragon, C., Balta-zar, G., Rehman, A. M., Matias, A., … Kleinschmidt, I. (2011). Determinants of bed net use in children under five and household bed net ownership on Bioko Island, Equatorial Guinea. Malaria Journal, 10(1), 179. https://doi.org/10.1186/1475-2875-10-179
- Hwang, J., Graves, P. M., Jima, D., Reithinger, R., Kachur, S. P., & Group, and the E. M. W. (2010). Knowledge of Malaria and Its Association with Malaria-Related Behaviors—Results from the Malaria Indicator Survey, Ethiopia, 2007. PLOS ONE, 5(7), e11692. https://doi.org/10.1371/journal.pone.0011692
- Mutuku, F. M., King, C. H., Mungai, P., Mbogo, C., Mwangangi, J., Muchiri, E. M., … Kitron, U. (2011). Impact of insecticide-treated bed nets on malaria transmission indices on the south coast of Kenya. Malaria Journal, 10, 356. https://doi.org/10.1186/1475-2875-10-356
- Owusu Adjah, E. S., & Panayiotou, A. G. (2014). Impact of malaria related messages on insecticide-treated net (ITN) use for malaria prevention in Ghana. Malaria Journal, 13, 123. https://doi.org/10.1186/1475-2875-13-123
- Schumacher, R.-F., & Spinelli, E. (2012). Malaria in Children. Mediterranean Journal of Hematology and Infectious Diseases, 4(1), 2012073.
- Somandjinga, M., Lluberas, M., & Jobin, W. R. (2009). Difficulties in organizing first indoor spray programme against malaria in Angola under the President’s Malaria Initiative. Bulletin of the World Health Organization, 87, 871–874. https://doi.org/10.2471/BLT.08.052514
- USAID. (2016). Angola, Malaria Operational Plan FY2016. Retrieved from https://www.pmi.gov/docs/default-source/default-document-library/malaria-op-erational-plans/fy16/fy-2016-angola-malaria-opera-tional-plan.pdf?sfvrsn=6
- Walker, P. G. T., Griffin, J. T., Ferguson, N. M., & Ghani, A. C. (2016). Estimating the most efficient allocation of interventions to achieve reductions in Plasmodium falciparum malaria burden and transmission in Africa: a modelling study. The Lancet Global Health, 4(7), e474–e484. https://doi.org/10.1016/S2214-109X(16)30073-0
- Weinstein, N. D. (1988). The precaution adoption process. Health Psychology, 7(4), 355–386. https://doi. org/10.1037/0278-6133.7.4.355
- World Health Organization. (2011). World health statistics 2011. Geneva: World Health Organization.
- World Health Organization. (2015). WHO | World Malaria Report 2015. Retrieved March 9, 2018, from http://www.who.int/malaria/publications/world-malar-ia-report-2015/report/en/
- Xu, J., Liao, Y., Liu, H., Nie, R., & Havumaki, J. (2014). Use of Bed Nets and Factors That Influence Bed Net Use among Jinuo Ethnic Minority in Southern China. PLoS ONE, 9(7). https://doi.org/10.1371/journal. pone.0103780
